Thyroid Deficiency Strikes One in Six
McDougall Newsletter - December 2005
Hypothyroidism is the most common of all the �hormone diseases,�
yet most people who have it are unaware. The test for this
deficiency is simple and almost painless, and the treatment is
effective, safe, and inexpensive. Left unattended, a subtle
malfunction could mean heart disease and an earlier death. With only
a slight decrease in thyroid hormone activity there are no symptoms;
however, because this gland affects the function of almost every
tissue in the body, severe deficiency can cause coma with
multi-system failure.
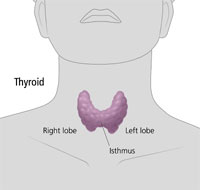 Hypothyroidism can be the result of iodine deficiency,
medications, surgery, and radiation, but the most common cause in
Western populations is a person�s own immune system attacking his
own thyroid gland. The inflammatory process is known as autoimmune
thyroiditis (also called Hashimoto�s thyroiditis after the doctor
who first described the condition in 1912). The results: 5-15% of
the general population, and as many as 20% of women, middle aged and
older, have a noticeable loss of thyroid function. The cause is
considered to be unknown, but as with other autoimmune diseases
(type-1 diabetes, rheumatoid arthritis, multiple sclerosis, etc.),
the rich Western diet is the likely source. (The immune system is
tricked by animal proteins that people consume to attack their
pancreas, joints, brain, thyroid and other tissues by a process
known as molecular mimicry.)
Hypothyroidism can be the result of iodine deficiency,
medications, surgery, and radiation, but the most common cause in
Western populations is a person�s own immune system attacking his
own thyroid gland. The inflammatory process is known as autoimmune
thyroiditis (also called Hashimoto�s thyroiditis after the doctor
who first described the condition in 1912). The results: 5-15% of
the general population, and as many as 20% of women, middle aged and
older, have a noticeable loss of thyroid function. The cause is
considered to be unknown, but as with other autoimmune diseases
(type-1 diabetes, rheumatoid arthritis, multiple sclerosis, etc.),
the rich Western diet is the likely source. (The immune system is
tricked by animal proteins that people consume to attack their
pancreas, joints, brain, thyroid and other tissues by a process
known as molecular mimicry.)
Diagnosis by a Simple Blood Test
Hypothyroidism may be suspected when people complain of fatigue,
weight gain, depression, slow mental processing, muscle weakness,
constipation, and/or feeling cold. However, these are symptoms
commonly seen with other conditions, including generally poor
health. Because the presentation is so nonspecific, anyone who does
not feel well should automatically have their thyroid status
checked.
Hypothyroidism is diagnosed by measuring a hormone produced by
the pituitary gland, called thyroid stimulating hormone (TSH). As
the name implies, this hormone stimulates the thyroid to synthesize
more hormones�and when the thyroid gland fails to respond as
directed, then more stimulating hormone is released in an attempt to
correct the deficiency. Thus an elevation of TSH means
hypothyroidism. Normal TSH levels are generally considered between
0.4 and 4.0 mU/L. Some authorities recommend lowering the upper
limits of normal to 2.5 mU/L, because levels higher than this could
mean more heart disease.1a
Before committing someone to a lifetime of thyroid replacement
therapy (pills), the TSH level should be repeated�after all, the
laboratory instruments could have been incorrectly calibrated that
day or your specimen could have been mixed up with someone else�s.
Treatment of Hypothyroidism
For most otherwise healthy adults with hypothyroidism, the
initial dose of thyroid replacement should be an amount equivalent
to 0.125 mg daily of levothyroxine. Lower starting doses may be
necessary for people with severe coronary artery disease. TSH levels
should be monitored every 4 to 6 weeks and appropriate adjustments
in dose made based on results. Using the results from blood tests, I
try to keep the TSH levels of my patients between 0.5 and 2.0 mU/L.1a
Once the correct dose is determined, then the TSH level should be
checked annually, unless the patient�s health suggests otherwise.
Even though treatment may seem simple, about one-fifth of patients
receive too little and one-fifth receive too much replacement with
thyroid medication.

Should Mild Hypothyroidism Be Treated?
Most doctors believe that slight decreases in thyroid hormone
production, seen by an increase in TSH level into the range of 2.5
mU/L to10 mU/L, should be left untreated.2 However, I hold a
�minority opinion� on this issue and often recommend treatment for
these laboratory results for several reasons. Many people with a
mild elevation of TSH go on to develop definite hypothyroidism�early
supplementation will prevent them from becoming clinically
hypothyroid, if and when their condition progresses. Treatment of
mild deficiency has been shown to relieve troublesome symptoms, like
fatigue and muscle dysfunction, and improve mental performance. 3,4
However, the most important reason that I treat mild elevations
of TSH is to reduce the risk of future coronary artery (heart)
disease. People with elevated TSH levels have higher cholesterol
levels and treatment with thyroid hormone supplements will lower
their total and LDL cholesterol levels.3,4 This elevation of
cholesterol associated with a slightly higher TSH level translates
into an increased risk of heart disease due to blocked coronary
arteries.5 Treatment has been found to reduce thickenings in the
walls of the arteries�a condition associated with a higher risk of
heart attacks and strokes.6 Mild hypothyroidism is associated with
an increased risk of congestive heart failure among older adults.7
Finally, the overall risk of death may be increased by a mild
decrease in thyroid activity as reflected in a slight elevation of
TSH.5
Is levothyroxine alone sufficient treatment?
It has been claimed that patients with hypothyroidism show
greater improvements in mood and brain function if they receive
treatment with Armour thyroid rather than Synthroid (levothyroxine).8
This conclusion is based on a 1999 study published in the New
England Journal of Medicine that actually tested a synthetic mixture
of levothyroxine (T4) and triiodothyronine (T3), rather the
pig-derived Armour preparation.9 The study showed some of the
measures for mental performance, mood and physical status were
improved in people taking the combination of both forms of thyroid
hormone, rather than the single hormone, levothyroxine. Such a
revelation caused quite a stir in the medical community because
doctors are traditionally taught that using levothyroxine alone is
the best way to treat hypothyroidism.
In response, several studies were performed to try to verify
these findings. Contrary to the New England Journal of Medicine
study, each of the newer studies failed to find an improvement in
mood or mental performance with the combination over single hormone
therapy.1a, 10-15 One study reported a higher risk of overdosing
patients�causing hyperthyroidism accompanied by feelings of impaired
well-being�due to the fast-acting T3 mixed in with the
preparation.11 Considering all of the research to date,
levothyroxine (the single hormone) alone should remain the treatment
of choice for replacement therapy of hypothyroidism.14 (There is
some pharmaceutical industry money funding this conclusion, so as
always, I reserve my right to change my opinion on drug therapy.)
Some of the reasons for caution are because of its quick onset
and short duration of action T3 can cause rapid and irregular
heartbeats and be difficult to monitor. All of the T3 we require is
naturally produced in our body from T4�the tissues slowly and safely
make a metabolic conversion of some of the T4 to T3.
Animal Extracts May Not Be Safe
Many patients I see express a desire for �natural therapies.�
Therefore, it should be no surprise to hear that they want to avoid
taking synthetic thyroid (levothyroxine); and instead request a
�natural� preparation, like the Armour brand. Extracts made from the
glands of animals contain several forms of the thyroid molecule,
including T3 and T4�and some doctors consider this an advantage,
while most research does not support this viewpoint.
The original treatment of hypothyroidism developed back in 1891
was made from extracts from the thyroid glands of sheep. Since then
the desiccated glands of other animals, including cows and pigs,
have been used. The process of making this medication begins with
removing the animal�s thyroid gland, then drying it, and finally
grinding it into a powder. Because of variations in concentrations
of active hormones in the animal�s glandular tissues the potency of
the preparations can vary greatly�people have developed serious side
effects from natural thyroid products that contained
greater-than-expected amounts of T3. Because of the �foreign� animal
tissues used natural thyroid supplements can also cause
�allergic-type� reactions, especially in people known to be allergic
to animal proteins.
One potential problem that has received no serious investigation
is the risk of contracting infection from consuming glandular
tissues in pill-form. Much work has been done showing animal-borne
microbes can be spread to people by eating animals as food16,17�and
there is every reason to believe the same can occur when dried
animal tissues sold as medications are consumed. Cancer, including
leukemia, viruses and AIDS-like viruses are commonly found in cows
and pigs.18-,19 These viruses are known to infect people.20 Could
these supplements be an unintended media for the spread of prion-based
brain diseases, like mad cow disease? There are many reasons to
believe that this is a real risk.21,22
The deadly H5N1 strain of bird flu has recently been found in pig
populations.23 History may be repeating itself. The deadly human
influenza virus of 1918 that killed more than 20 million people
worldwide was a mutation of a swine flu virus that evolved from
American pigs and was spread around the world by US troops.24
Since there has been essentially no effort by the livestock
industry in most (but not all) countries to clean up their animals,
hundreds of different kinds of infectious microbes are being
consumed by billions of people. Therefore, to protect yourself and
family there is every good reason to not eat these animals and their
byproducts, including glandular extracts, like �natural� thyroid
extract. (For more information see my February 2004 newsletter
article: Widespread Infection with Leukemia Virus from Meat and
Milk.)
Overdosing By Self-medicating and the �Natural� Doctor
In my practice I often see patients who are taking an overdose of
thyroid medication. They may be self-medicating in hopes of feeling
more energetic or losing weight effortlessly. Another real
possibility is their doctor, often referred to as �alternative,
holistic, and/or complementary,� prescribes a supraphysiologic dose
to treat various ailments, such as chronic fatigue syndrome or
arthritis.
In actual practice, people almost never require more than 0.2 mg
of levothyroxine (equal to about 2 grains of thyroid extract). In
addition to failing to resolve health and weight problems, too much
thyroid can result in bone loss and heart arrhythmias.25,26
A Change in Diet Will Not Correct Hypothyroidism
Once the thyroid tissue is destroyed it will not regrow and I
know of no way to stimulate the remaining gland to work harder. Many
people ask if avoiding cruciferous vegetable foods or taking extra
iodine will cure their thyroid condition. Compounds in plant foods,
like cabbage, cauliflower, Brussels sprouts, millet and soy have
antithyroid effects. These foods are referred to as goitrogenic
foods because theoretically they can lead to a condition of low
thyroid with an associated gland enlargement, called a goiter.
Supplementation with iodine completely reverses the goitrogenic
influence of any vegetables. (Incidentally, these same foods have
compounds that protect against thyroid cancer.27)
There is no harm in trying to improve your thyroid function by
avoiding cruciferous vegetables, soy and millet, and/or adding more
iodine (like from sea vegetables) to your diet, but my experience
has been that this effort will make no difference. Let me know if
you find otherwise.
Simple, Safe, Effective Medical Care
Part of the routine evaluation of all of my patients is a check
of their thyroid status. If their TSH levels are above 3 mU/L (after
two separate tests), then I consider recommending supplementation
with levothyroxine. I lean more towards treatment the higher the TSH
level (the more severe the hypothyroidism). Also, if they have a
higher risk for heart disease, then I am more inclined to recommend
treatment.
Even though I have not found the benefits to be great, I am
sometimes persuaded to treat when weight loss or fatigue is the
patient�s concern, and they also have a slightly abnormal TSH level.
Other times, when the decision to treat a slightly abnormal TSH
levels is not straight-forward, I may suggest a six month trial on
thyroid and look for subjective (feelings of well-being) and
objective (lower cholesterol) improvements.
Thyroid supplementation is one of the very few treatments I
commonly prescribe. (See my November 2004 newsletter for a more
complete list of McDougall-used medications.) For my patients with a
damaged thyroid gland, correcting hypothyroidism with the right
amount of levothyroxine can be an inexpensive medical miracle
without side effects.
References:
1a: Spencer CA. Demers LM. LMPG: Laboratory Support for the
Diagnosis and Monitoring of Thyroid Disease (Published Guidelines):
http://www.nacb.org/lmpg/thyroid/3c_thyroid.doc
1) Dong BJ, Hauck WW, Gambertoglio JG, Gee L, White JR, Bubp JL,
Greenspan FS. Bioequivalence of generic and brand-name levothyroxine
products in the treatment of hypothyroidism. JAMA. 1997 Apr
16;277(15):1205-13.
2) Crapo LM. Subclinical hypothyroidism and cardiovascular
disease. Arch Intern Med. 2005 Nov 28;165(21):2451-2.
3) Roberts CG, Ladenson PW. Hypothyroidism. Lancet. 2004 Mar
6;363(9411):793-803.
4) Ayala AR, Wartofsky L.The case for more aggressive screening
and treatment of mild thyroid failure. Cleve Clin J Med. 2002
Apr;69(4):313-20.
5) Imaizumi M, Akahoshi M, Ichimaru S, Nakashima E, Hida A, Soda
M, Usa T, Ashizawa K, Yokoyama N, Maeda R, Nagataki S, Eguchi K.
Risk for ischemic heart disease and all-cause mortality in
subclinical hypothyroidism. J Clin Endocrinol Metab. 2004
Jul;89(7):3365-70.
6) Monzani F, Caraccio N, Kozakowa M, Dardano A, Vittone F,
Virdis A, Taddei S, Palombo C, Ferrannini E. Effect of levothyroxine
replacement on lipid profile and intima-media thickness in
subclinical hypothyroidism: a double-blind, placebo- controlled
study. J Clin Endocrinol Metab. 2004 May;89(5):2099-106.
7) Rodondi N, Newman AB, Vittinghoff E, de Rekeneire N,
Satterfield S, Harris TB, Bauer DC. Subclinical hypothyroidism and
the risk of heart failure, other cardiovascular events, and death.
Arch Intern Med. 2005 Nov 28;165(21):2460-6.
8) Use Armour thyroid rather than Synthroid: http://www.mercola.com/1999/archive/armour_thyroid.htm
9) Bunevicius R, Kazanavicius G, Zalinkevicius R, Prange AJ Jr.
Effects of thyroxine as compared with thyroxine plus
triiodothyronine in patients with hypothyroidism. N Engl J Med. 1999
Feb 11;340(6):424-9.
10) Escobar-Morreale HF, Botella-Carretero JI, Gomez-Bueno M,
Galan JM, Barrios V, Sancho J. Thyroid hormone replacement therapy
in primary hypothyroidism: a randomized trial comparing L-thyroxine
plus liothyronine with L-thyroxine alone. Ann Intern Med. 2005 Mar
15;142(6):412-24. (Merck sponsored).
11) Siegmund W, Spieker K, Weike AI, Giessmann T, Modess C,
Dabers T, Kirsch G, Sanger E, Engel G, Hamm AO, Nauck M, Meng W.
Replacement therapy with levothyroxine plus triiodothyronine (bioavailable
molar ratio 14 : 1) is not superior to thyroxine alone to improve
well-being and cognitive performance in hypothyroidism. Clin
Endocrinol (Oxf). 2004 Jun;60(6):750-7. (No sponsor listed)
12) Clyde PW, Harari AE, Getka EJ, Shakir KM. Combined
levothyroxine plus liothyronine compared with levothyroxine alone in
primary hypothyroidism: a randomized controlled trial. JAMA. 2003
Dec 10;290(22):2952-8. (Sponsor, National Naval Medical Center)
13) Sawka AM, Gerstein HC, Marriott MJ, MacQueen GM, Joffe RT.
Does a combination regimen of thyroxine (T4) and
3,5,3'-triiodothyronine improve depressive symptoms better than T4
alone in patients with hypothyroidism? Results of a double-blind,
randomized, controlled trial. J Clin Endocrinol Metab. 2003
Oct;88(10):4551-5. (Sponsored by Aventis)
14) Escobar-Morreale HF, Botella-Carretero JI, Escobar del Rey F,
Morreale de Escobar G. REVIEW: Treatment of hypothyroidism with
combinations of levothyroxine plus liothyronine. J Clin Endocrinol
Metab. 2005 Aug;90(8):4946-54 (Sponsored by University Grants)
15) Walsh JP, Shiels L, Lim EM, Bhagat CI, Ward LC, Stuckey BG,
Dhaliwal SS, Chew GT, Bhagat MC, Cussons AJ. Combined thyroxine/liothyronine
treatment does not improve well-being, quality of life, or cognitive
function compared to thyroxine alone: a randomized controlled trial
in patients with primary hypothyroidism. J Clin Endocrinol Metab.
2003 Oct;88(10):4543-50. (Sponsored by Sir Charles Gairdner Hospital
Research Foundation)
16) zur Hausen H. Proliferation-inducing viruses in
non-permissive systems as possible causes of human cancers. Lancet.
2001 Feb 3;357(9253):381-4.
17) Talbot SJ, Crawford DH. Viruses and tumours--an update. Eur J
Cancer. 2004 Sep;40(13):1998-2005.
18) Burny A, Cleuter Y, Kettmann R, Mammerickx M, Marbaix G,
Portetelle D, van den Broeke A, Willems L, Thomas R. Bovine
leukaemia: facts and hypotheses derived from the study of an
infectious cancer. Vet Microbiol. 1988 Jul;17(3):197-218.
19) Randal J. Xenografts raise questions about cancer virus
transfer to humans. J Natl Cancer Inst. 1998 Feb 18;90(4):264-5.
20) Buehring GC, Philpott SM, Choi KY. Humans have antibodies
reactive with Bovine leukemia virus. AIDS Res Hum Retroviruses. 2003
Dec;19(12):1105-13.
21) Castilla J, Gutierrez-Adan A, Brun A, Doyle D, Pintado B,
Ramirez MA, Salguero FJ, Parra B, Segundo FD, Sanchez-Vizcaino JM,
Rogers M, Torres JM. Subclinical bovine spongiform encephalopathy
infection in transgenic mice expressing porcine prion protein. J
Neurosci. 2004 May 26;24(21):5063-9.
22) Bradley R. The research programme on transmissible spongiform
encephalopathies in Britain with special reference to bovine
spongiform encephalopathy. Dev Biol Stand. 1993;80:157-70.
23) Bird flu in pigs: http://news.bbc.co.uk/1/hi/world/asia-pacific/3601798.stm
24) Pigs carried 1918 flu: http://www.lubbockonline.com/news/032197/1918flu.htm
25) Quan ML, Pasieka JL, Rorstad O. Bone mineral density in
well-differentiated thyroid cancer patients treated with suppressive
thyroxine: a systematic overview of the literature. J Surg Oncol.
2002 Jan;79(1):62-9.
26) Sawin CT, Geller A, Wolf PA, Belanger AJ, Baker E, Bacharach
P, Wilson PW, Benjamin EJ, D'Agostino RB. Low serum thyrotropin
concentrations as a risk factor for atrial fibrillation in older
persons. N Engl J Med. 1994 Nov 10;331(19):1249-52.
27) Tadi K, Chang Y, Ashok BT, Chen Y, Moscatello A, Schaefer SD,
Schantz SP, Policastro AJ, Geliebter J, Tiwari RK.
3,3'-Diindolylmethane, a cruciferous vegetable derived synthetic
anti-proliferative compound in thyroid disease. Biochem Biophys Res
Commun. 2005 Nov 25;337(3):1019-25.

